As of January 1st, 2022, the HealthWatch CCM team started utilizing MDRevolution (MDR) software to document all CCM visits and capture patient billing. iSalus built an integration to MDR in order for clients to receive their CCM documents and claims directly into their databases. This article outlines commonly asked questions about the integration and any updates you should expect with this new software.
Q. Do I have to do any setup in my database to activate the integration?
A. No! Our team took the responsibility of ensuring all databases were setup and ready for the integration. You will now see a new user in your database named "MDR Integration," this is required in order to activate the API. We ask that you please do not deactivate or change the password for this user, this will disrupt the integration and will not allow your notes/claims to come through. You also have a new user group called "CCM Escalation Team," this will be explained further in the Q&A. There will also be a new order bluebar and an enrollment screen within patient setup, also explained in more detail further into the Q&A.
Q. When can I expect my CCM notes and claims to appear in my database?
A. Encounters now close on the last day of the month, whereas before they were closed immediately after the call. This allows our team to keep the note open throughout the month, capturing the additional conversations and minutes spent coordinating care for each patient. We often spend more than 20 minutes assisting the patient throughout the month and MDR allows us to capture that time. Due to this improvement, all notes and claims will be available in your billing portal and patient charts between the 5th - 8th of the following month.
Q. Where do I find my CCM claims, has anything changed?
A. Nothing has changed for claims processing, besides timing! Your CCM claims will continue to directly flow into your billing portal, in your list of closed claims. You can expect each all claims to appear on the 5th-8th business day of the month following the prior month close (i.e. for January, all claims should appear around the 5th of February).

Q. Where do I find my CCM visit notes, has anything changed?
A. There are two differences in the CCM visit notes:
- Previously you located your CCM visit notes on the timeline under "Health Exchange," the only difference moving forward is notes will now be in eDocuments. Each month your CCM visit notes will be distributed to the Patient Documents cabinet, within the CCM Visit Notes drawer, in the CCM Visit Notes folder. You can access these from the patient timeline, eDocuments in the patient chart, or the eDocuments portal.
- Our notes have a new layout! Previously our SOAP notes were overloaded with excess information, making it difficult for the Provider to identify the most important information from the visit. Our new notes display the most pertinent questions/information at the top of the note, organized in an encounter note based on the timeline in which the care was coordinated. Patient escalations and vitals, when provided, are also visible in a timeline within the CCM note.
Q. How will patient escalations and patient requests be handled with the integration?
A. With our new integration we have the ability to send the practice messages directly from the patient chart in MDR to a CCM escalation team at the practice. We will utilize this method to send patient appointment requests, medication refill requests/questions, lab questions, any escalations the patient had during a visit, and whatever else the patient has requested/any information the practice needs to know about the visit. There is now a "CCM Escalation Team" user group in your database, we suggest you assign your dedicated team members to this user group, they will be the front line in assisting with any patient care coordination.

Q. How can I tell if a patient is enrolled or opted out of the program?
A. You can view your patients eligibility and enrollment status from Patient Setup. Go to Patient Setup, then open the Miscellaneous section, you will see your patient status under "MDRevolution Status." As we enroll and discharge your patients, their status will automatically update.
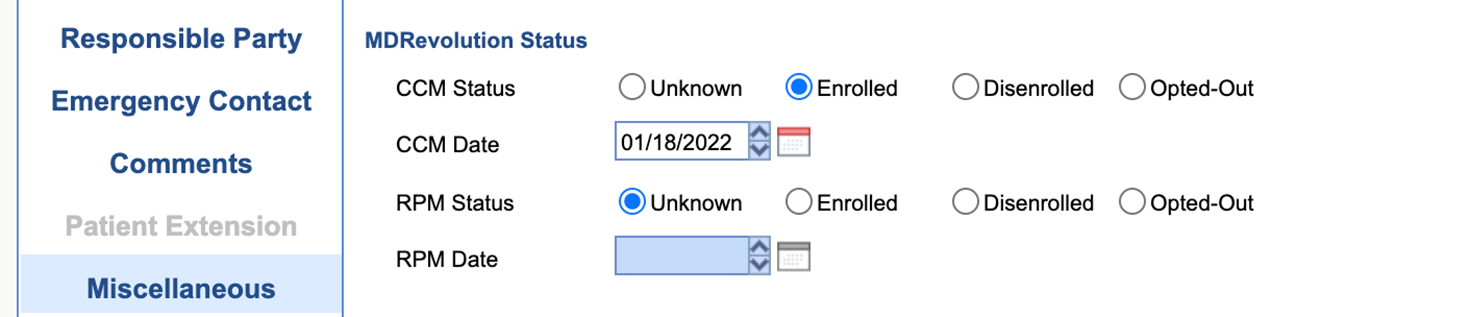
Q. How do I order CCM for a patient?
A. There will be two options for ordering patients within iSalus:
- Eligible patients will continue to be automatically identified through our pop health algorithm, if you're accustomed to ordering patients from the Pop Health MyTask screen, you can continue to do so.
- Providers/Clinical Staff now have the option to order CCM for patients directly from the patient chart! The clinical team will order CCM like they order any other lab/service. A new bluebar will be added for CCM services, and the practice should complete the same workflow they do for lab/radiology integrations. More to come on this workflow very soon!
Q. What deems my patient eligible for CCM services?
A. Patients with multiple (two or more) chronic conditions expected to last at least 12 months or until the death of the patient, and that place the patient at significant risk of death, acute exacerbation/decompensation, or functional decline, are eligible for CCM services. Examples of chronic conditions include, but are not limited to, the following:
- Alzheimer’s disease and related dementia
- Arthritis (osteoarthritis and rheumatoid)
- Asthma
- Atrial fibrillation
- Benign prostatic hyperplasia (BPH)
- Cancer
- Cardiovascular Disease
- Depression
- Diabetes
- Hypertension
- Overactive Bladder Disorder (OAB)
- Prostate Cancer
Q. How do I order CCM services for a patient? (iSalus Software Customers)?
A. Follow the below instructions:
- Login to your database and from the MyTask list, click into the Pop Health MyTask
- If you are a rendering provider (or a staff member who is responsible for working the queue on behalf of a rendering provider) and do not see any patients listed, make sure your user setting is set to rendering provider:
- Click on your username in the bottom left hand corner of the screen to open user setup
- From user setup, make sure the correct username is selected on the left-hand side, then click the icon that has the red-shirted character to open advanced settings
- Once the advanced user settings screen appears, in the setting search bar search “chronic,” then click on the “Population health Settings 2” setting that appears
- From the Pop Health setting, from the Provider dropdown, select the appropriate rendering provider, once selected click the floppy disk to save the top toolbar
- If you would like to see a list of all eligible patients, regardless of rendering provider, type a % sign in the search bar and click the search icon (magnified glass)
- Once you have the appropriate list of patients, to order a patient for CCM:
- Select the patient you would like to order from the list, you’ll see all their information in regard to their CCM eligibility on the right-hand side once they’re selected.
- In the bottom right hand corner click “Order CCM”
- You will be prompted to confirm the rendering provider, then click yes or no to order the patient
- If you would like to order without having to confirm, you may select “Don’t show this message again,” which will remove this pop-up moving forward.
Q. How do I notify HealthWatch that a patient would like to discharge from the program?
A. You can submit a patients request to discharge from the program through this link: https://app.smartsheet.com/b/form/31c8ff9dbe0243a3acb9d854b2e8b96c
Q. How does HealthWatch gain consent for CCM services?
A. The patient is contacted by our patient care coordination team, where they are explained the program. Once they understand the program they are asked if they would like to consent to setting up their first CCM appointment. The patient is walked through cost sharing, who HealthWatch is, and why they are eligible for the program. Again, at the end of the discussion, their consent is confirmed.
Q. What is my patient consenting to?
A. Patients consent to receiving care coordination through monthly check-in calls with a medical assistant, and mail care coordination.
Q. Does HealthWatch use scripting when gaining patient consent?
A. Yes, each patient care coordinator is provided scripting to speak with each patient. They follow basic guidelines to ensure the patient is provided all necessary information on the program but will also work with each individual to answer any questions they may have. The PCC is there to help the patient understand the benefits of the CCM program and how they can take advantage of their Medicare benefits.
Q. Is a new patient consent required each calendar month, or annually?
A. No, a new consent is only required if the patient changes billing practitioners, in which case a new consent must be obtained and documented by the new billing practitioner prior to furnishing the service
Q. Is a written consent required?
A. No, CMS does not require written consent be obtained to enroll patients into the CCM program, a verbal consent is allowed.
Q. What should my patients expect when receiving care coordination from HealthWatch?
A. Patients can expect to receive care coordination one of two ways:
- Monthly calls - we strive to coordinate a mutual time to speak with the patients. At that time, our staff contacts each patient on the phone and spends 20 minutes every month discussing their care plan and progress toward the patient’s individual healthcare goals.
- Mailed care coordination – some patient request to receive their monthly CCM services via mail, with their consent we will deliver the following materials via mail: patient education (differs each month), a paper medical exam to complete, a medication list to complete and a return envelope and stamp to return their care coordination items. This is all documented in the clinical note within the patient’s chart.
Q. How is the care coordination documented?
A. Each visit is documented in a patient specific care plan, whether the patient received care coordination over the phone or through the mail. This care plan becomes a locked medical note, which lives in their HealthWatch chart.
Q. What does my patients care plan consist of?
A. The medical care coordination team will conduct care coordination with the patient each month, which includes, but is not limited to, the following:
- Reconciling of medications and medication education
- Health questionnaire – we utilize a very detailed condition management care plan to review the patients general health and chronic condition progression, any additional chief complains from the patient during the visit are also documented (urology, nephrology, cardiology, mental health, general health, neurology, COVID-19). We are happy to share a copy of this care plan with the practice at any time
- Care Plan Review
- Patient Education – unique to each visit
Q. What else do you do to help coordinate care for my patients outside of their standard monthly visit?
A. We strive to help patients with as much as possible, a few examples include:
- Medication refills to the practice and the pharmacy
- Appointment scheduling and management to other specialists, PCP, etc.
- DME Supply coordination (Blood pressure monitors, walkers, CPAP machines, etc.)
- Call on the patient’s behalf to receive their imaging and lab results
- Schedule appointments with the practice for follow-up
- If a patient notes they went to the ER/were hospitalized, we call the practice(s) to schedule a follow-up appointment
- Coordination transportation for the patient as needed
Q. Do you have testimonials from patients on their experience with HealthWatch CCM?
A. Yes! We are in the process of building a landing page on our HealthWatch website where you can find great feedback from our CCM patients. We also share patient testimonials regularly with our customers as we receive them from our patients.
Q. What are the details and requirements for billing a 99490 code?
A. Chronic care management services, at least 20 minutes of clinical staff time directed by a physician or other qualified health care professional, per calendar month, with the following required elements:
- Multiple (two or more) chronic conditions expected to last at least 12 months, or until the death of the patient
- Chronic conditions place the patient at significant risk of death, acute exacerbation/ decompensation, or functional decline
- Comprehensive care plan established, implemented, revised, or monitored
Q. How does billing the Add-On Code 99439 work?
A. CMS recognized there is a significant gap of time and resources between 99490 and 99487, therefore they created the 99439 code. 99439 is meant to reimburse clinicians for all 20-minute increments of time spent on patients, after the first 20-minutes. This first 20-minutes is still coded as 99490.
- Up to two 99439 codes can be added to 99490 in a month.
- Like 99490, 99439 cannot be used in conjunction with 99487, 99489, or 99491.
Q. How much does CCM cost to the patient?
A. With the patient being a Medicare beneficiary, Medicare will pay for this service, once the patients annual deductible is met. Their secondary insurance should cover the 20% ($10-$14) copay, alleviating any out of pocket cost to the patient. As the billing practitioner, you should be filing both the Medicare and secondary insurance for these services.
- There are 3 secondary insurances who will not cover the copay for CCM. There insurances are Humana, Tricare and Optima Health. Any patients who have one of these as a secondary insurance will be liable for the $8 copay for every completed Chronic Care Management exam. *Patients must have Medicare as their primary insurance.
- Only one in 10 beneficiaries relies solely on the Medicare program for health care coverage. The rest have some form of supplemental converge to help with medical expenses, so approximately 90% of patients may not have to pay out of pocket for the co-pays.
Q. Do Medicare Advantage (MA) plans reimburse for CCM? What about commercial payers?
A. A Medicare Advantage plan is required to offer its enrollees at least traditional Medicare benefits, which now will include CCM. It seems reasonable to assume that an MA plan will pay for CCM just as it now pays for other physician services. Whether commercial payers will pay for CCM remains to be seen, although the fact that CMS is paying for this service makes it more likely.
Q. How do I reconcile the CCM patients I was invoiced for by HealthWatch?
- Login to your database and go to the Billing portal
- From the billing portal, on the left-hand side, under “Insurance” click “Billing Query”
- Under search criteria, “Claim,” in the “Code(s)” field, enter “99490,” then under the “Procedure” section, set your “Post Date” based on your invoice month (example below would be an invoice from August)
- Once your criteria is set, click the magnified glass in the top toolbar to bring back your search results.
- The total number of rows displayed in the bottom left hand corner of the search screen should match your invoice number, so in this example, you would have been invoiced for 2006 patients.
- If for some reason your invoicing is off, please contact your HealthWatch point of contact.
Q. How do I handle patient billing disputes?
A. At times, a patient may feel as if they were billed incorrectly for a CCM service (i.e. did not understand there would be a fee, feel they did not consent, etc.). If a patient communicates with the practice about disputing their CCM charge, it is at the discretion of the practice to refund the patient. If the practice would like more information to make this decision, they should follow these steps:
- Gather the patient’s information, their dispute, and submit a review form: https://app.smartsheet.com/b/form/dfacac83646b42729d9ed9e310691ab9
- The form will be submitted to the HW management team where they will evaluate the patients phone encounters, CCM medical notes, exam history, and listen to any recordings related to the billing concern.
- The HW management team will then connect back with the practice to deliver findings on the dispute. The practice can then reconnect with the patient and decide whether to refund the claim.
- If the HW team finds the patient received care coordination incorrectly at the fault of the HW staff, the practice will be notified, and they will receive a credit from HealthWatch on their next invoice. The practice will be credited their contracted rate.
Q. How do I handle my practice claim disputes/questions?
A. If a practice receives a CCM claim denial and would like HealthWatch to review the denial, or potentially seek credit for the denial, they should follow these steps:
- The practice has 60 days from the CCM date of service to dispute any claims and/or invoicing issues, this can be referenced on your HealthWatch monthly invoice:
- Input patient’s information, their dispute/claim denial reason and submit a review form: https://app.smartsheet.com/b/form/dfacac83646b42729d9ed9e310691ab9
- The form will be submitted to the HW management team where they will evaluate the patients phone encounters, billing, CCM medical notes, exam history, and listen to any recordings related to the billing concern.
- The HW management team will then connect back with the practice to deliver findings on the claim denial.
- The HW team will work with the practice to explain the denial reasoning, and assist them in getting the claim updated to be resent if applicable
- The practice should then reconnect with the patient and decide whether to refund the claim or reprocess the claim if it was a failed claim and it can be resubmitted.
Q. Why may a credit need to be rendered?
A. Below are a few examples a credit may be provided to the practice from HealthWatch:
- Patient is deceased – it is (unfortunately) common for a patient to pass away while they are enrolled in CCM and for the HealthWatch team to not be notified until after they have sent the patient care coordination via mail. Patients receive monthly calls, and if they do not answer their routine monthly call, our HealthWatch team will send them their care coordination in the mail. Once the practice is notified of the passing, they should alert the HealthWatch immediately so the patient can be discharged.
- Patient was hospitalized – similar to the deceased example, patients may become hospitalized while enrolled in the CCM program. Once the HealthWatch team is notified, the patient will be discharged, or placed on hold, and the patient can be credited for the care coordination they received while in the hospital.
- Patient was enrolled in another CCM program – our care coordination team always asks our patients if they are enrolled in another CCM program, but sometimes the patient does not understand they’re in another program or they were not informed. If a patient is enrolled in two CCM programs, the practice claim may be denied and listed as “too many frequency of services.” In this case we would credit the practice for the HealthWatch CCM charge and discharge the patient from our program.
*THIS PAGE IS UNDER CONSTRUCTION FOR CERTAIN SECTIONS, MARKED WITH AN ASTERISK.
Q. How do I know if my patient is enrolled in HW CCM (iSalus Software Customers)?
- A. You can view your patients eligibility and enrollment status from Patient Setup. Go to Patient Setup, then open the Miscellaneous section, you will see your patient status under "MDRevolution Status." As we enroll and discharge your patients, their status will automatically update.

Q. How do I access the claims sent to my system (iSalus Software Customers)?
- To work claims from the Billing wheel:
- Go to the Billing portal
- Click on the red “Prepare” section, and once you options appear, click into “Ready for Processing,” then if there are CCM claims to be processed you will see the option “Closed – Electronic CCM,” click that option to open all unprocessed CCM claims in the billing query
- To see any unworked, pending CCM chargers:
- Go to the Billing portal
- From the Billing portal, under Insurance, click on Billing Query
- From the search criteria window, under the “Claim” section, from the status dropdown select “closed electronic – CCM,” then, if needed, you can set a service range and several other data fields.
- Once you have all fields set, click the magnified glass in the top toolbar to search, this will put back any unworked CCM claims.
- To see CCM charges that have already been processed or CCM charges across all time:
- Go to the Billing portal
- From the Billing portal, under Insurance, click on Billing Query
- From the search criteria window, under the “Claim” section enter the code “99490” in the “Code(s)” field
- If you choose you can set a date range for this search as well under the section “Procedure”
- Once you have all fields set, click the magnified glass to pull back all CCM claims
*Q. How do I access the claims sent to my system (Non-iSalus Software Customers)?
- Go to the Billing portal
- From the Billing portal, under Insurance, click on Billing Query
- From the search criteria window, under the “Claim” section, from the status dropdown select “closed electronic – CCM,” then, if needed, you can set a service range under the “Procedure” section.
- Once your search criteria are set, click the magnified glass in the top toolbar to bring back all results.
- Once all results are loaded, to export, click the manilla folder icon, and click “Excel Export”
*Q. How often are claims sent?
A. If you have an integration, claims are the billing portal between the 5th-8th of the month following the prior month close. If you do not have integration, your claims will be sent to you via sftp or through a secure Box account between the 5th-8th.
*Q. How do I access my patient’s HealthWatch CCM notes?
- Login to your database
- Go to the EMR portal
- Open the chart of the patient who you would like to review their CCM note (If you are not opening from a scheduled appointment, search for the patient in the top right-hand corner of the EMR)
- Once you have opened the patient’s chart, the first screen to appear will be the summary chart tab, this is where you will access the HW notes.
- From the summary chart tab, on the bottom of the screen, reference the patient timeline, under the row “HealthExchange” you will see a record of all your completed HW notes
- Click on the note, this will open a separate window, then double click on the HW note to open and review details from the HW care coordination
*Q. How often are notes sent?
A. Notes are sent immediately to the practices database once signed off in the HW database and can be access from the summary chart tab on the patient’s timeline, under the “HealthExchange” section.





















